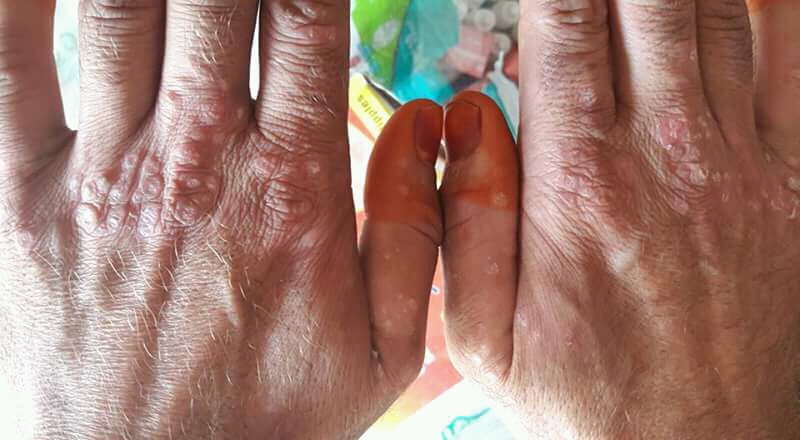
The key symptoms of Psoriasis are: Well-demarcated, raised red plaques covered with thick silvery-white scale, classically on the elbows, knees, scalp, and lower back; lesions are symmetric and persist for months to years., Pinpoint bleeding when scale is scraped off — the Auspitz sign — caused by tortuous dilated capillaries in the dermal papillae just beneath the thinned epidermis., Itching of moderate intensity in roughly 70-90% of patients; less prominent than in eczema but often interferes with sleep., Burning, stinging, or soreness within active plaques, especially in flexural psoriasis or sensitive sites like the genitals., Cracking of plaque skin with painful fissures, particularly over the knuckles, palms, and soles; bleeding fissures are common in palmoplantar disease., Nail changes including pitting (small depressions in the nail plate), onycholysis (lifting of the nail), oil-drop spots, and subungual hyperkeratosis — present in 50% of patients., Scalp involvement with thick, scaly plaques that extend beyond the hairline onto the forehead, retroauricular skin, and posterior neck; temporary diffuse hair shedding can occur..
01Well-demarcated, raised red plaques covered with thick silvery-white scale, classically on the elbows, knees, scalp, and lower back; lesions are symmetric and persist for months to years.
02Pinpoint bleeding when scale is scraped off — the Auspitz sign — caused by tortuous dilated capillaries in the dermal papillae just beneath the thinned epidermis.
03Itching of moderate intensity in roughly 70-90% of patients; less prominent than in eczema but often interferes with sleep.
04Burning, stinging, or soreness within active plaques, especially in flexural psoriasis or sensitive sites like the genitals.
05Cracking of plaque skin with painful fissures, particularly over the knuckles, palms, and soles; bleeding fissures are common in palmoplantar disease.
06Nail changes including pitting (small depressions in the nail plate), onycholysis (lifting of the nail), oil-drop spots, and subungual hyperkeratosis — present in 50% of patients.
07Scalp involvement with thick, scaly plaques that extend beyond the hairline onto the forehead, retroauricular skin, and posterior neck; temporary diffuse hair shedding can occur.
08Koebner phenomenon — new plaques developing 7-14 days after skin trauma, surgical incisions, tattoos, or sunburn — present in 25-30% of patients.
09Joint pain, stiffness, and swelling (especially morning stiffness lasting >30 minutes), dactylitis (sausage digits), and enthesitis — features of psoriatic arthritis in 30% of skin-disease patients.
10Psychological burden including depression, anxiety, and reduced quality of life that often exceeds the burden of comparable medical conditions; suicidality risk is elevated.