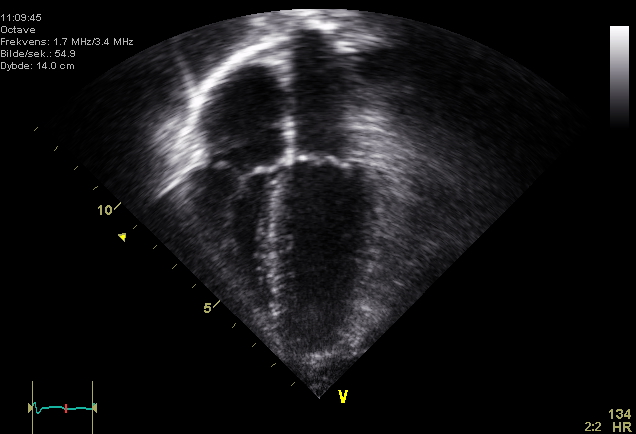
- Coronary artery disease and prior myocardial infarction
- Ischemic cardiomyopathy is the leading cause of HFrEF in high-income countries. Myocardial infarction destroys functioning muscle and triggers maladaptive remodeling. About two-thirds of HFrEF cases worldwide have an ischemic etiology.
- Long-standing hypertension
- Chronically elevated afterload produces left ventricular hypertrophy, diastolic stiffness, and ultimately systolic decline. Hypertension is the leading single risk factor for HFpEF and the second-leading for HFrEF after coronary disease.
- Valvular heart disease
- Severe aortic stenosis, aortic regurgitation, mitral regurgitation, and mitral stenosis all impose pressure or volume overload that culminates in heart failure. Valve surgery or transcatheter intervention can reverse the syndrome early in the course.
- Cardiomyopathies (dilated, hypertrophic, restrictive)
- Genetic and acquired myocardial diseases produce systolic or diastolic dysfunction independent of coronary disease. Dilated cardiomyopathy is the most common HF cause in patients under 60; titin and lamin gene variants are increasingly identified.
- Atrial fibrillation with rapid ventricular response
- Sustained tachycardia (>110 bpm for weeks) causes tachycardia-induced cardiomyopathy in some patients. Rate or rhythm control can fully reverse HF in this subgroup.
- Diabetes, obesity, and metabolic syndrome
- Obesity and type 2 diabetes drive both HFrEF and especially HFpEF through microvascular disease, myocardial lipid accumulation, systemic inflammation, and AGE-mediated stiffening. They roughly double HF lifetime risk.
- Cardiotoxic drugs and substances
- Anthracycline chemotherapy (doxorubicin), trastuzumab, certain tyrosine kinase inhibitors, immune checkpoint inhibitors, methamphetamine, cocaine, and heavy chronic alcohol use cause cardiomyopathy. Risk is dose-related and often partially reversible if recognized early.
- Myocarditis and infiltrative disease
- Viral myocarditis (Coxsackie B, parvovirus, SARS-CoV-2), sarcoidosis, amyloidosis (especially ATTR in older men), and hemochromatosis can produce restrictive or dilated phenotypes. Cardiac MRI and targeted testing identify these.